Leukopathy is a neurological disorder characterized more precisely by a lesion of the white matter whatever the cause of the lesion.
Leukopathy comes from the Greek leuco = white and from pathos = disease.
Leukoencephalopathy is also a medical term used by the physicians.
Most of the time, it is accompanied by blood circulation problems in the brain. The latter is then poorly irrigated by the arterioles and capillaries. We speak of leukopathy (or vascular leukoencephalopathy).
What is white matter?
White matter is part of the nervous tissue made up of axons. Axons are extensions of neurons that allow information to pass between two neurons by propagating nerve impulses .
They are surrounded by a myelin sheath, a lipid layer (made of cholesterol, phospholipids and glycolipids.
White matter is therefore involved in the transmission of information in the central nervous system and the brain in particular.
The myelin sheath is therefore damaged in leukopathy.
Axon surrounded by a myelin sheath. This sheath is damaged in vascular leukopathy
Classification of different types of leukopathy
A distinction is made between acquired leukopathies and those which are hereditary.
Hereditary leukoencephalopathies having a genetic cause are then classified according to the gene which is involved (this gene mutates and this mutation is at the origin of the lesion of the white matter).
As for acquired leukopathies, they are classified into different groups according to their underlying causes:
- inflammatory and non-infectious.
- inflammatory and infectious.
- hypoxic and ischemic. (example Binswanger’s disease)
- traumatic.
- toxic and metabolic.
Examples of diseases that lead to leukopathy
There are several diseases that lead to white matter damage :
Multiple sclerosis
The multiple sclerosis is a neurological disease characterized by inflammation of neurons (called neuroinflammation).
Progressive multifocal leukoencephalopathy
Progressive multifocal leukoencephalopathy (PML) is a rare, often fatal neurological disorder characterized by nerve cell destruction caused by the JC virus. It has been associated mainly with hematological malignancies and organ transplant recipients, but the number of cases has increased significantly due to the use of immunosuppressive drugs. Common symptoms include cognitive dysfunction, hemianopsia, aphasia, motor or sensory dysfunction, seizures and ataxia. PML starts as an asymptomatic persistent infection in the kidney and may spread to other organs through contact with an infected individual or contaminated food or water. The syndrome was particularly common among people with HIV/AIDS in the 1980s, but its occurrence has increased significantly since then due to the wider use of immune-modulating drugs such as natalizumab and efalizumab.
Leukoaraiosis
Leukoaraiosis is also accompanied by neuroinflammation.
Alzheimer’s disease
The Alzheimer’s disease is the most important form of dementia and is accompanied by abnormalities of the white matter.
Toxic leukoencephalopathy
It is a rare condition characterized by progressive damage to the white matter caused by drug addiction, environmental toxins, or chemotherapy drugs. The severity of toxic leukoencephalopathy also varies depending on the patient, the duration of exposure and the concentration of the toxic agent. The disease may be reversible in many cases when the toxic agent is removed.
Reversible posterior leukoencephalopathy syndrome
Posterior Reversible Encephalopathy Syndrome (PRES) is a syndrome characterized by headache, confusion, seizures and loss of vision. It can have several causes, including malignant hypertension and certain medical treatments. On magnetic resonance imaging (MRI) of the brain, there are areas of edema (swelling). Symptoms tend to go away after a while, although sometimes visual changes remain.
Hypertensive leukoencephalopathy
Hypertensive leukoencephalopathy refers to a degeneration of the white matter of the brain following a sudden increase in blood pressure. People may experience a sudden increase in blood pressure, an acute confusional state, headache, vomiting, and seizures. Retinal hemorrhages may be present during the examination. Hypertensive leukoencephalopathy can lead to cardiac ischemia.
Along with these acquired leukoencephalopathies, there are those which originate from a genetic mutation:
Megalencephalic leukoencephalopathy with subcortical cysts. This form of leukopathy has a genetic cause. It is characterized by subcortical cysts (small cavities). It belongs to a group of diseases called leukodystrophies. (also called Van der Knaap disease).
Diffuse hereditary axonal spheroid leukoencephalopathy
Leukoencephalopathy with neuroaxonal spheroids is a special form of leukoencephalopathy. Spheroids are discontinuous axonal swellings characterized by the absence of myelin sheaths. They cause progressive cognitive and motor regression. It is a disease of genetic origin, following an autosomal dominant profile . It usually presents in childhood, but it can also appear in adulthood, in which case it can have neurological features similar to those of multiple sclerosis.
Hereditary vascular leukoencephalopathies
They include CADASIL disease (NOTCH3 gene mutation), CARASIL disease (HTRA1 gene mutation) and cerebral amyloid angiopathy. In the case of CADASIL, there is a family history of cerebral stroke.
Childhood Ataxia with diffuse Central nervous system Hypomyelination
This syndrome was initially described in children. The adult forms
are however more and more recognized. The neurological symptoms are very variable (cerebellar ataxia, psychiatric and dementia symptoms). It is an autosomal recessive neurological disease, caused by mutation of EIF genes. This disease belongs to the leukodystrophies family.
How to screen for vascular leukopathy?
Brain imaging exams (MRI, scanner) make it possible to detect leukopathies. These leukopathies result in lacunae (small cavities that reflect damage to the central nervous system), small bleeding and damage to the outer capsules of the white matter.
Leukopathies generally affect people with vascular risk factors (with a risk of vascular dementia), with cardiovascular problems or suffering from atherosclerosis. These are, for example, people with diabetes, hypertension and high cholesterol.
It is possible that individuals who are free of any of the diseases described below and under the age of 50 may develop leukopathy. In this case, the diagnosis will be based on a genetic disease such as leukodystrophy, also called genetic leukoencephalopathy.
Leukoencephalopathies of genetic origin include hereditary diseases characterized by a disease of the white matter:
- vascular leukoencephalopathies such as CADASIL disease and familial cerebral amyloidosis.
- Ataxia with Central nervous system hypomyelanisation.
- Fragile X syndrome with early gait disturbances.
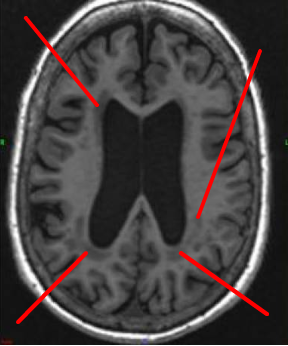
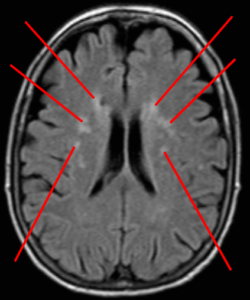
The consequences of leukopathy
Leukopathy increases the risk of stroke, cognitive impairment (memory, executive functions), movement coordination disorders or seizures.
