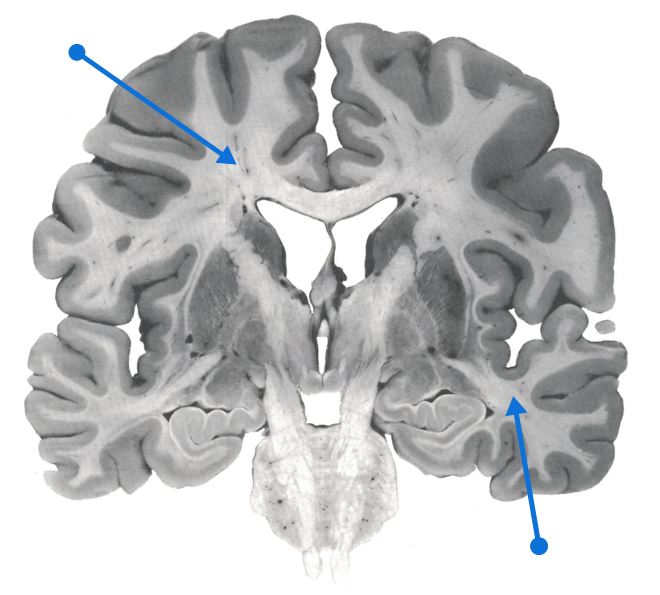
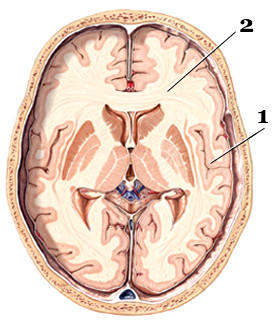
White matter is the part of the tissue of the central nervous system (including the brain and spinal cord) that mainly contains extensions of neurons.
These extensions called axons are surrounded by a myelin sheath which is the origin of this whitish structure, as well as glial cells which nourish and protect the nerve cells.
The myelin is a fat which protects the fibers and gives color to the white matter.
It also ensures rapid propagation of information in the nervous system in the form of an electrical signal. These lesions are characterized by damage to the tissues located in the deepest part of our brain, due to health problems associated with aging. This tissue contains millions of axons, which connect other parts of the brain and spinal cord.
White matter lesions
Lesions from this substance are common in the elderly, especially in those with a history of hypertension and cerebral deficiencies.
Many diseases, injuries, and toxins can cause white matter changes:
- Long-term high blood pressure
- Inflammation of the blood vessels
- Tobacco consumption
Controlling hypertension well
The results showed that individuals with white matter lesions more often had a history of hypertension (+ 270%), compared to those without lesions. They also had a much larger number of brain deficiencies (+ 448%).
Cognitively, patients with these types of lesions performed poorer on cognitive tests, suggesting that this category of people has an even greater risk of developing Alzheimer’s disease.
« Our results report a correlation between white matter lesions and impaired cognitive functions, suggesting that these lesions worsen this deficit in individuals with mild cognitive impairment. »
Consequently, it is advisable to control the cardiovascular risk factors at the origin of these lesions, in particular hypertension, and to a lesser extent diabetes, hypercholesterolemia and atheroma.
It remains to be determined whether these lesions increase the conversion rate between mild cognitive impairment and dementia.
Source: Duron E. et al. Relations between cognitive disorders and lesions of the cerebral white matter. Archives of diseases of the heart and vessels. 100 (8), 2007.
Symptoms
- Learning and memory disabilities: difficulty learning or remembering new things
- Difficulty solving problems
- Incontinence
- Depression
- Walking disorders
- Balance disorders with risk of falls
People with damage to white matter – the part of the brain made up of the axons of neurons – have an increased risk of stroke and dementia such as vascular dementia or Alzheimer’s disease. It is possible to prevent and slow down this damage.
White matter lesions increase risk of stroke
A meta-analysis comprising twenty-seven studies that compared healthy older people to those with cognitive impairment caused by white matter damage.
White matter lesions affect small blood vessels deep in the brain, unlike Alzheimer’s disease which narrows the hippocampus, causing progressive loss of memory.
The disease hardens the small arteries and gradually limits the arrival of nutrients in the white matter, leading to a loss of several cognitive functions: planning, organization, problem solving, attention, working memory, immediate and delayed memory.
These conditions increase a person’s risk of having a stroke and even of developing dementia such as vascular dementia or Alzheimer’s disease.
“Our results support the idea that white matter lesions gradually alter the brain and cognitive functions, without modifying activities of daily living », declared the author of a study published in 2014.
White matter damage increases risk of Alzheimer’s
In 2004, a Dutch study involving more than a thousand subjects followed for 5 years already indicated that white matter (WM) damage quadrupled the risk of dementia, including Alzheimer’s type dementia ( Prins et al., Arch Neurol., 61: 1531- 4 ).
It is estimated that 5 percent of Canadian adults have a vascular cognitive impairment, possibly related to hypertension , high cholesterol , poorly controlled diabetes, poor dietary hygiene, inactivity and smoking.
WM damage is anatomically characterized by arteriosclerosis, myelin damage and activation of glial cells (gliosis). They are caused by an ischemic attack which affects the small arteries.
The good news is that WM damage can be reduced by adopting healthy lifestyle habits that reduce the risk of heart attack and stroke.
Source: The neuropsychological profile of vascular cognitive impairment not demented: A meta-analysis. Journal of Neuropsychology, février 2014.
In another study, American researchers reported white matter and gray matter damage in people aged 40. This damage is subsequently associated with a decline in cognitive functions, or even with Alzheimer’s disease.
The study’s author, Dr. Pauline Maillard, explained that the study shows for the first time that hardening of the arteries harms the brain and that the problem manifests itself in midlife, much earlier than did not anticipate it.
Worsening of cognitive impairment
White matter lesions, common in older people with hypertension, may be responsible for mild cognitive impairment.
Another study determined whether the presence of WM damage was associated with a more marked decline in cognitive performance in individuals with mild cognitive impairment, a sometimes transient state between normal cognitive functioning and dementia. Almost 15% of people with mild cognitive impairment (MCI) develop dementia per year.
136 patients – diagnosed with mild cognitive impairment – underwent a battery of neuropsychological tests * and a neurological examination (CT scan) to determine the presence of lesions.
* Mini-examination of mental state and cognitive efficiency profile
These patients were on average 75 years old, of whom more than half had hypertension (54%) and a third had white matter lesions. Hypertension was characterized by a pressure greater than 140/90 mmHg.
How are they diagnosed?
A magnetic resonance imaging ( MRI ) test can show any damage. White matter changes appear to be very bright (referred to as a « hyper-intense » signal) during an MRI scan.