Alzheimer’s disease is responsible for several symptoms (i.e. what the patient feels) and is characterized by clinical signs that can be observed by relatives and the doctor.
Some warning signs are often insidious: changes in weight, behavior, language, walking, and sleep, as well as the occurrence of repeated falls.
Signs and Symptoms of Alzheimer’s Disease
Recent memory loss
Memory problems are the symptoms that constitute the main reason for consultation, on the initiative of the patient or more frequently that of the family. Indeed, the patient tends to minimize or deny his troubles. Memory difficulties relate to recent facts and then to old facts. It is the so-called episodic memory that is mainly affected. For example, people with Alzheimer’s disease will often forget to go to an appointment (if it is a frequently recurring event). According to a study published in 2015, women with memory trouble have an increased risk (+70%) of developing dementia from the age of 65.
Difficulties performing daily tasks
People will have difficulty performing familiar everyday tasks that do not require special effort (eg using a household appliance).
Difficulty expressing oneself and finding the right words.
A person with Alzheimer’s disease often forgets simple words. For example, she will ask for « the thing to eat » rather than the fork.
Difficulty orienting oneself in space and time.
The person with Alzheimer’s disease can get lost in their own street, no longer know where they are and no longer be able to return home.
Difficulties in passing judgment.
People with Alzheimer’s can dress without paying attention to the outside temperature. In addition, they lack discernment in matters of money and may be victims of abuse.
Difficulties in handling abstract notions.
A person with Alzheimer’s disease loses track of numbers or what they represent. For example, she doesn’t know what the numbers on a bank statement or a street sign represent.
Difficulty finding lost items.
A person with Alzheimer’s disease will store things in an inappropriate place. For example, keys in a fridge or a watch in a shoebox.
Depressive and behavioral disorders.
A person with Alzheimer’s can quickly change mood and go from a serene state to crying or angry outbursts, for no apparent reason. Numerous studies have even shown that nearly 90% of patients suffering from Alzheimer’s disease also present with mood disorders, agitation, and loss of appetite. According to their authors, these results suggest that these disorders occur years before the diagnosis of dementia. Patients with Alzheimer’s disease also presented behavioral problems earlier: loss of appetite, apathy, irritability, etc.
Personality changes.
A person with Alzheimer’s can quickly become very confused, fearful or suspicious of someone close to them.
Loss of interest. The person with Alzheimer’s may become passive and spend hours doing nothing (eg watching television for hours, sleeping more than normal, and not going outside).
In summary, Alzheimer’s disease results in cognitive and non-cognitive (ie psychological and behavioral) symptoms that impair activities of daily living.
The two forms of Alzheimer’s disease symptoms
Symptoms can be divided into two classes: cognitive symptoms and psychological and behavioral symptoms.
Cognitive symptoms
Memory problems: the person has problems retrieving information stored in their brain. This incapacity is compensated for at the start of the disease thanks to the work of certain parts of the brain which
remain intact (in particular the frontal lobe), but is gradually accentuated as the disease worsens.
Initially limited to the years preceding the disease, retrograde amnesia gradually spreads until reaching the earliest memories and even the identity of the patient, who has more and more difficulty recognizing his relatives. Amnesia affects both episodic memory (the patient’s own memories) and semantic memory (knowing how to name objects or images, having verbal fluency, etc.). Working memory is generally impacted at the onset of the disease: patients have difficulty performing simultaneous tasks.
Semantic memory deficits generally occur later than episodic memory disorders. This translates into difficulty in saying as many words as possible beginning with a given letter (poor verbal fluency), in making paraphasias (e.g. saying table instead of desk), in responding in a more general way (by say animal for dog) and to experience problems of categorical classification (the patient has trouble guessing which of the fir tree or the palm tree is semantically closest to the pyramid).
Visual and spatial disorders
Language disorders: they are linked to semantic memory disorders and can be early. At the beginning of the disease, they are most often characterized by a lack of words which alters spontaneous speech: patients often try to circumvent the obstacle by using circumlocutions. At this stage there is generally no phonemic or syntactical disturbance or comprehension disturbances and speech is normal. At a more advanced stage, paraphasias are numerous. We observe perseverations on a word or a syllable, or around a theme. Logical word order disappears in speech, and listening comprehension is disrupted. On the other hand, written language can be affected, with spelling difficulties.
Finally, in the severe stage of the disease, spontaneous production is greatly reduced, or even non-existent. It may be limited to echolalia. The language is misunderstood. This is called global aphasia.
Practical disorders (apraxia)
Loss of recognition of objects, faces (agnosia) .
Impaired executive functions and judgment. Disorders of executive functions are manifested by difficulties in abstraction, reasoning, mental flexibility and planning.
Psychological and behavioral symptoms
- Depressive symptoms
- Loss of initiative and interest
- Indifference
- Anxiety, often associated with depression.
- Irritability
- Hustle
- Aggressive
- Delusions (ideas of persecution, jealousy)
- Hallucinations (mainly visual)
- Sleeping troubles
- Wanderings (severe stage)
- Runaways
- Confusional episodes (in moderate and severe stages).
- Disinhibition
- Repetitive motor behaviors
- Eating Disorders
What are the signs that should worry us?
There are reasons for concern when a person:
- cannot do two things at once (e.g. cook dinner);
- wanders off on a familiar path;
- forgets the names of relatives;
- no longer recognizes the faces of relatives;
- rehashing the same questions.
A consultation is necessary if the person:
- no longer knows how to perform certain daily tasks (eg operate a washing machine);
- gets lost in family ties;
- no longer knows the function of certain objects;
- puts things away in inappropriate places.
On the other hand, there is no cause for concern when the person:
- no longer knows where she parked her car;
- forgets to call someone back;
- forgets the name of a person she has just met;
- no longer knows where to put an object;
- can’t remember a word.
Other possible warning signs
Anosognosia
Patients suffering from Alzheimer’s disease have little or no awareness of their disease: this is called anosognosia . It complicates patient care and increases the caregiver’s burden. This would be one of the possible warning signs.
Mild behavioral disorder (deficit): one of the precursor symptoms of Alzheimer’s disease
Researchers have compiled a list of behavioral symptoms to help identify those at risk, assuming that certain behavioral changes may be a warning sign of Alzheimer’s disease. Experts have long emphasized that mild cognitive impairment is an early warning sign of Alzheimer’s disease. Now, some of them are pushing a new concept they call “mild behavioral (deficit) disorder,” describing persistent abnormal changes in an older person’s behavior. Changes include issues such as social withdrawal, tantrums, anxiety, and obsession.
“We are not talking about a jolt in someone’s behavior but about abnormal and persistent behavior. it would be the first sign that something is wrong in the brain,” says the lead author of the study.
He and his colleagues developed a symptom checklist that doctors could use to assess patients with behavioral problems. The tool needs to be refined, however, as the research presented at the Alzheimer’s Disease Conference is preliminary.
“People often think that Alzheimer’s disease is primarily a problem of memory loss. However, many patients with dementia also have neuropsychiatric symptoms – an umbrella term encompassing behavioral problems and mood and perceptual disturbances”.
According to the researcher, it is important for doctors that families can realize that lasting changes in behavior can be a warning sign.
Here is a list of symptoms of mild behavioral disorder:
- decreased motivation which refers to apathy or a lack of interest in things in which individuals had an interest. For example, a grandparent no longer seems interested in the lives of his grandchildren. Apathy appears in 25% to 50% of patients, depending on the study;
- emotional symptoms such as depression, anxiety and irritability;
- difficulty controlling impulses that manifests as restlessness, obsession, or even habits like gambling;
- problems with perception, with the presence of delusions or hallucinations. Older people have a mild behavioral problem if they have any of these symptoms, periodically, for at least six months.
Researchers estimate that 13% of older people with mild cognitive impairment will develop dementia within a year. This percentage rises to 25% if there is also the presence of mild behavioral problems.
Currently, there are no treatments that can prevent or permanently treat the symptoms of Alzheimer’s disease. However, early detection allows for available treatments and support services as soon as possible. When it comes to behavioral issues, there are ways to deal with them. In some cases, a minor change in a person’s environment can help. Some people can be treated with medications such as antidepressants or anti-anxiety medications under the supervision of a doctor. Source: Alzheimer’s Association International Conference, Toronto, July 2016.
In 2015, a study conducted by American researchers (Washington University School of Medicine, Saint-Louis) already indicated that behavioral disorders could be present before memory problems. The authors describe these disorders with, in order of appearance:
- irritability,
- depression,
- sleep disturbances,
- anxiety,
- change in appetite,
- restlessness and apathy,
- exaltation,
- motor disorders,
- hallucinations,
- the illusions and
- disinhibition.
To reach this conclusion, the authors of the study analyzed the files of 1218 people who had initially consulted without signs of Alzheimer’s disease, before the latter does not start thereafter. Source: “Noncognitive” symptoms of early Alzheimer disease. Neurology, January 2015.
However, a study published in JAMA Psychiatry in 2017 does not support the idea of personality change before the onset of mild cognitive impairment or dementia.
According to the lead author of the study:
We found that the personality remained stable even in the last years before the onset of the disease.
The researchers analyzed the personality and cognitive performance of more than 2,000 individuals who had no cognitive deficit before the study. About 18% of study participants later developed cognitive impairment or dementia.
What the researchers found was that the trajectory of personality traits did not differ between those who would later develop dementia and those who remained without cognitive problems.
While personality change was not an early sign of dementia, the study further supports the fact that personality traits (eg high emotionality or low level of conscientiousness) are risk factors for dementia. Source: A. Terracciano et al. Personality Change in the Preclinical Phase of Alzheimer’s Disease. JAMA Psychiatry, September 2017.
Oral expression
American researchers have tried to detect the first signs and symptoms of Alzheimer’s disease in Ronald Reagan, by studying his press conferences when he was President of the United States of America. The texts have been compared to those of George HW Bush Sr. Responses to press conferences have the particularity of requiring a significant cognitive effort because they must be spontaneous.

Ronald Reagan was diagnosed with Alzheimer’s in 1994, five years after he left the presidency of the United States. He had been regularly followed by his doctors during his two presidential terms. His remarks made during public conferences have in particular been closely scrutinized. For example, during a debate with his opponent W. Mondale in 1984, he had confused the place where was with the federal capital (Editor’s note which can be seen as a slip). Arizona State University researchers noticed subtle changes between his first and second terms when they compared excerpts from his press conferences with those of George HW Bush, the two being around the same age. at the beginning of their mandate (69 years old for Reagan in 1981, 64 years old for Bush in 1993). Using an algorithm, they studied the changes in the modes of expression of the two presidents. This algorithm had been used to analyze novelists’ writing changes.
Results: Ronald Reagan tended, towards the end of his presidency, to repeat the same word and to use imprecise words (example “thing”), contrary to his successor George Bush who did not develop Alzheimer’s disease.
The researchers point out, however, that this algorithm should be tested on a large number of people in order to validate it scientifically. As a reminder, difficulties in finding the right words are one of the main warning signs of the disease. Thus, a person with Alzheimer’s disease no longer remembers simple words (“eg knife”) and will replace them with an expression (“the thing to cut”). This is difficult to detect at the onset of the disease, because the patient masks his condition by using carefully repeated sentences and simple words. This algorithm had previously been used on the writings of Agatha Christie, suspected of having suffered from Alzheimer’s disease, as well as on those of the British writer Iris Murdoch, suffering from the disease.
Alzheimer’s: altered signs in brain activity
A French study (Pitié-Salpêtrière, Paris, France) aims to identify early the first signs and symptoms of Alzheimer’s disease in 400 people aged 70 and under and in good mental health. Participants will have to pass cognitive tests in the form of mental exercises. In parallel, the electrical activity of the brain – more precisely the cerebral cortex – is recorded by electroencephalography (EEG).
The slightest change in brain activity could be interpreted as a sign of a loss of synaptic connections and gray matter, characteristic of the onset of Alzheimer’s disease.
The interest of the study, called Insight, is therefore to identify the patient before he is in a prodromal state, that is to say before the first symptoms become detectable by neuropsychological tests. To do this, the researchers hope to be able to identify symptoms and warning signs of Alzheimer’s disease before the prodromal stage. The 400 participants will take cognitive tests every five years (twice a year) (memory, attention, executive functions, language, praxis, etc.).
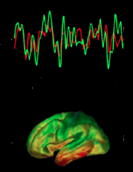
Neuropsychologists try to distinguish the disorders that normally appear during aging from those that should alert, in particular the difficulty of memorizing a newly acquired word or a new event (we speak of anterograde amnesia). While performing their mental exercises, researchers place electrodes on individuals’ skulls to perform an EEG. According to the researchers, “Alzheimer’s disease alters the EEG at rest and during exercise. These subtle changes are the consequence of a loss of neurons and synapses (areas of contact between neurons). A blood test will be taken at the same time.
When a case of Alzheimer’s has declared itself, the blood samples will be analyzed to identify biological markers likely to be involved in the pathology of the disease. Finally, the individuals are subjected twice a year to a magnetic resonance imaging (MRI) examination, which will make it possible to visualize any brain lesions, in particular in the hippocampus – an area involved in memory. It is estimated that the volume of the hippocampus decreases by more than 4% per year in Alzheimer’s patients, compared to only 1% in healthy subjects.
Slower walking
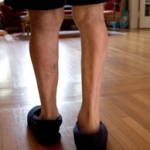
Older people who walk more slowly have higher amounts of amyloid in their brains, a French study has found. Researchers have reported an association (albeit a modest one) between higher levels of amyloid plaques in the brain and slower walking speed in older adults. Amyloid is a protein that accumulates – in the form of plaques – in the brain of Alzheimer’s patients.
« These results suggest that people with Alzheimer’s disease show subtle signs of gait disturbances, in addition to well-known symptoms such as memory complaints, even in those with a normal gait rhythm, » said Dr. lead author of the study (University of Toulouse).
This study, which allowed researchers to look at participants at a specific point in time, only established an association between brain amyloid levels and walking speed, but not a causal relationship between the two. The research team analyzed 128 people (average age: 76) who had no formal diagnosis of dementia, but were considered high risk due to memory problems. Almost half had abnormally high levels of amyloid plaque in their brains (48%) and mild cognitive impairment (46%). Gait speed was measured using a standard synchronization test (transition from brisk walking to usual walking pace). Amyloid accumulates in several regions of the brain,
“The way we walk is controlled by areas of the brain that define rhythm. When this part of the brain does not work properly, it can have an impact on walking or speed, ”explains an Alzheimer’s disease specialist.
However, it is important to reassure older people who walk slower than others. In 2012, American researchers (Boston Medical Center) also studied the association between walking and cognitive performance in 2,140 volunteers aged 62 on average. They had started from the hypothesis that difficulty in walking and walking speed are warning signs of symptoms characteristic of Alzheimer’s disease. Their results reported a link between walking speed and the onset of dementia. This association has to date no scientific explanation. Source: Del Campo N et al. MAPT/DSA Study Group. Relationship of regional brain β-amyloid to gait speed. Neurology. 2016 Jan 5;86(1):36-43.
Alzheimer’s: brain imaging to confirm the symptoms of Alzheimer’s disease
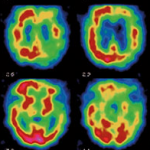
Signs of brain damage can appear well before the first symptoms in healthy individuals whose parents both have Alzheimer’s disease.
“When the diagnosis is made, it is already too late,” says Dr. Lisa Mosconi (New York University School of Medicine). “This is why it is necessary to detect the signs of the disease in these people at risk before the first symptoms”.
52 subjects aged 32 to 72 underwent neuroimaging examinations – including positron emission tomography and magnetic resonance imaging – which visualize amyloid plaques and brain activity.
Results: Individuals whose parents had Alzheimer’s disease had more amyloid plaques and a lower brain volume, compared to those whose parents had no pathology.
“Our study suggests the existence of predisposition genes that promote lesions characteristic of Alzheimer’s disease in individuals at risk. It remains to be determined which ones. Source: Brain imaging of cognitively normal individuals with 2 parents affected by late-onset AD. Neurology, 2014.
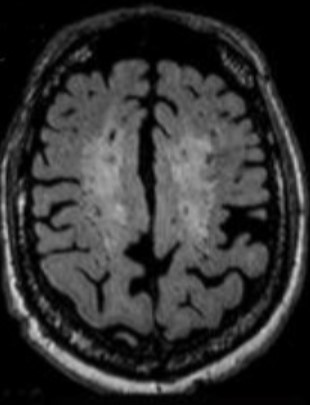
Analysis of the structure by MRI is characterized by atrophy in the temporal cortex (in particular the hippocampus) and the parietal cortex, with an accentuation of the sulci.
Imaging confirms or not the diagnosis of the presence of symptoms characteristic of Alzheimer’s disease and allows the doctor to decide to prescribe a drug.
Sleep problems

An experiment conducted on mice suggests that sleep disturbance could be one of the early signs of Alzheimer’s disease. In the study published in Science Translational Medicine (Sept. 2012), the researchers showed that the sleep cycle was disrupted when amyloid plaques appeared in the brains of these mice. As a reminder: amyloid plaques are characteristic lesions of Alzheimer’s disease; Researchers have succeeded for fifteen years in “manufacturing” transgenic mice which develop these lesions as they age. It is important to detect early warning signs of the disease well before the appearance of the first symptoms (loss of short-term memory).
« If sleep problems at the very beginning of the disease, these signs and symptoms could serve as a means of detecting Alzheimer’s disease », explains one of the authors of the study who adds: « we do not yet know in what form These sleep disorders appear: reduction in sleep time, difficulty in falling asleep…”.
Frequent falls
People with lesions characteristic of Alzheimer’s disease (deposits of amyloid plaques and tau proteins) see their risk of falling multiplied by 3 when they practiced an activity of daily living. These results come from an American study of 125 people (average age: 74 years) whose number of falls was evaluated for one year. Amyloid deposits and elevated levels of tau protein were measured in cerebrospinal fluid after lumbar puncture. Source: Neurology, July 30, 2013.
The causes that may explain these falls are numerous and associated with other signs and symptoms of Alzheimer’s disease:
- Deficit in cognitive faculties (judgment, attention).
- Loss of coordination and skill.
- Decline of sight.
- Malnutrition leading to loss of muscle mass.
- Fatigue related to wandering.
