Frontal subcortical dementia is a form of dementia characterized by attention disorders, slowed cognitive performance, severe dysexecutive syndrome, decreased verbal fluency and elaborate language, constructive apraxia (loss of ability to executing gestures or using objects, without any paralysis).
Practical case of frontal subcortical dementia
Mr. A. was diagnosed with Alzheimer’s disease upon entering a long-term care facility with a Mini-Mental State Examination (MMSE) score of 16/30.
His GMP is 850, which means he is very addictive. GMP stands for Weighted Average GIR. It corresponds to the average level of dependency of residents of a long-term care facility in France. The higher the GMP, the greater the level of resident dependency. Generally speaking, a GMP greater than 300 corresponds to a medical establishment. An establishment with a GMP greater than 700 corresponds to a geriatric hospital.
Long-term care takes care of elderly patients, the vast majority of whom have memory problems which are often the reason for their placement.
The medical staff suspected that the diagnosis made before the patient arrived at the facility was incorrect because his cognitive state was not deteriorating.
He continued to memorize names well, to orient himself well in space and to remember past events concerning him (autobiographical memory). In addition, he obtained a score of 20/30 on the MMSE five years after entering the establishment, an increase of 4 points.
A neuropsychometric assessment and a neuroimaging examination (magnetic resonance imaging) indicate that the pathology from which Mr. A. suffers is not characteristic of Alzheimer’s disease.
Neuropsychometric assessment
The patient’s cognitive performance declines only slightly, with mild time orientation disorder , episodic memory encoding and retrieval disorder, dysexecutive syndrome, mild selective attention deficit, mild apraxia ideomotor, as well as difficulties in performing mental calculations.
Neuroimaging examination: the diagnosis of subcortical frontal dementia is made
Presence of vascular lesions and atrophy of the hippocampus.
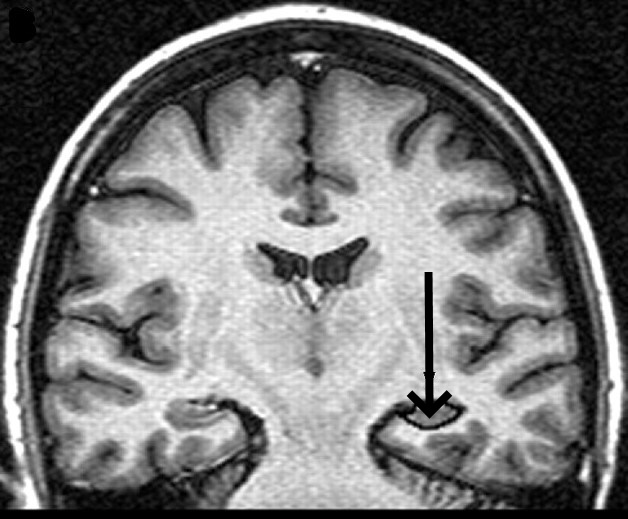
The diagnosis of Alzheimer’s disease remains therefore uncertain.
Symptoms are those seen in subcortical frontal dementia.
The patient continues to receive an acetylcholinesterase inhibitor type medicine (e.g. Aricept) and a platelet aggregation inhibitor.
